Fill form to unlock content
Error - something went wrong!
Submit the information below to access the paper.
Thank you!
Cut Bedside False Alarms Up to 99% with Real-Time Analytics
Even in the best of circumstances, the sensory overload of hospital bedside alarms causes undue stress and fatigue for healthcare workers. The flood of alerts, most without merit, means that the medical staff is less likely to respond. As a result, patient care suffers.
Continuous clinical surveillance can cut through the noise. By gathering and analyzing data from multiple sensors, these systems offer a more holistic view of patient health—sounding the alarm only when truly needed. This can extend the reach of ICU staff to better aid patients, wherever they receive care in the facility.
How many alarms are we talking about? In a 2006 study by Johns Hopkins Hospital conducted over 12 days recorded a total of 58,764 alarm conditions, or 350 alarm conditions per patient per day.
These numbers explain the high rate of alarm fatigue, in which doctors and nurses become inured to all of the warnings and alerts—no longer taking them seriously—even when a patient may be experiencing a life-threatening condition. The problem is so dire that the ECRI Institute labeled alarm fatigue as a number-one medical hazard.
While alarm fatigue is nothing new, it’s only getting worse. What’s changed? Technology is propelling use of monitoring devices, with an average of 10 to 15 per bed. A shortage of healthcare workers, combined with complex regulations, is increasing the stress on nurses, doctors, and their patients.
Patient monitoring devices are intended to improve medical outcomes. This can happen only when their data is integrated, analyzed, and acted on in real time. But constant monitoring can create havoc if systems are not properly managed.
Continuous Surveillance Goes Beyond Patient Monitoring
In essence, these separate medical devices capture and process a wide range of medical data from very sick patients and those recovering from major surgeries. But considered separately, the data can be overwhelming and difficult to take action on. To improve outcomes, clinicians and caregivers must receive timely alerts related to the patient’s condition—while avoiding false alarms—so that they can swiftly perform their duties.
A continuous-surveillance solution brings the data from these different devices together to help clinicians recognize a patient’s physiological trends. By pairing algorithms and predictive models at the edge with vital-sign data, changes in patterns can be detected. This includes:
- Automatically making sense of multiple data types such as heart rate, respiration rate, blood pressure, skin temperature, and more.
- Capacity to analyze changing patterns in clinical data over time.
- Applying rules-based data analytics to signal unexpected changes before a life-threatening situation occurs.
- Flexibility to network with any device and adapt to a wide range of clinical protocols.
Capsule has devised a system that provides this type of continuous surveillance. The Capsule Medical Device Information Platform collects medical device data and runs analytics on that information as shown in Figure 1.
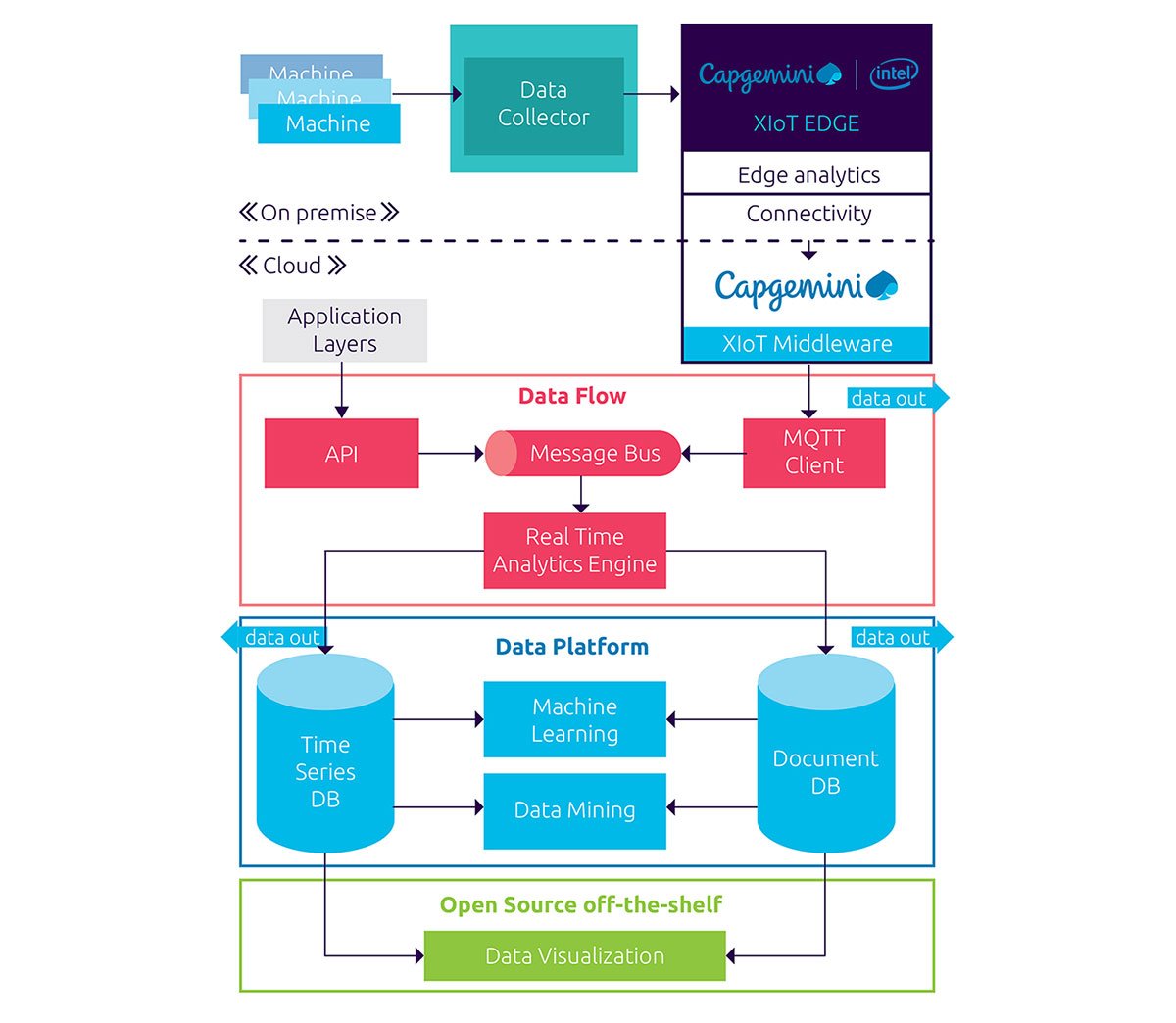
Real-Time Analytics at the Edge
The solution’s middleware detects pattern changes in oxygenation levels, heart rate, pulse rate, carbon dioxide level, and other metrics. It then applies that data in milliseconds to rules-based phenomenon algorithms.
Capsule’s low-latency technology helps provide clinicians with advance warning, so they can intervene and stabilize a patient as soon as deterioration is detected.
“What makes us different from basic alarm management systems is that we’re using real-time patient physiologic parameters coming from one or more devices,” said Janet Dillione, CEO of Capsule. “If that device is speaking every second, we're getting it every second. If it talks every minute, we see it every minute.”
Consider the difficulties of managing ventilator alarms—a top-of-mind priority for many facilities. The Capsule Ventilated Patient Surveillance application addresses this critical challenge. The system enables remote data access, making ventilated patient care safer and more efficient. With a centralized view, clinicians can better manage ventilated patients and associated alarm conditions while also reducing nuisance alarms.
Helping Patients Recover
As another example, major-surgery patients are often prescribed opioids for pain management, putting them at risk for opioid-induced respiratory depression (OIRD), in which a patient simply stops breathing.
“More than 20,000 patients per year experience OIRD,” said Dillione. “And opioids—while a powerful way to reduce chronic pain—are the cause of half of all medication-related deaths in hospitals,” Dillione added.
Furthermore, the enormous economic impact of OIRD accounts for nearly $2 billion a year in U.S. healthcare costs.
A recent clinical study showed that the Capsule Medical Device Information Platform reduced the number of OIRD false alarms by 99 percent. And the system enabled alerts 100 percent of the time when patients were approaching an episode.
“For this customer, in the first 30 days after Capsule platform went into production, they had reduced 23,000 alarms down to 200,” said Dillione. “We not only reduced the noise by 99 percent, but we've also identified the patients who are at tremendous risk.”
These remarkable results show how IoT technologies can have huge impacts on improving outcomes. When healthcare workers get the information they need, when they need it, patients are more likely to recover from major surgeries.
Flexible and Secure
The Capsule Medical Device Information Platform is a flexible and scalable solution, making it simple to configure without customization or rewriting code. The platform, which runs on Intel® technology, including Intel® Core™ and Intel® Xeon® processors, is FDA Class II approved for patient monitoring and secondary alarm management.
On top of this, the system adheres to the National Institute of Standards and Technology (NIST) Cybersecurity Framework, enabling hospitals to:
- Meet HIPAA compliance by providing security safeguards that ensure the integrity of electronic protected health information (ePHI).
- Assess and mitigate cybersecurity risks associated with malware, ransomware, and other threats to patient data.
- Identify and validate modifications to the platform and medical device security logs and settings.
“We take security very seriously. We have an ability to provide auditing for any change that's made on any device on any parameter,” said Dillione.
False alarms create stress for patients and hospital staff, and are clearly a significant problem. They interfere with the ability of clinicians to provide proper care to patients, often with serious consequences.
The bottom line is that the Capsule Medical Device Information Platform has been shown to reduce alarms by up to 99 percent, improving patient safety as well as bringing a better environment to healthcare workers, making their jobs a lot easier.